Published: December 2019
Last Reviewed: November 2025
Scars are a natural part of the body’s healing process, forming whenever the skin or deeper tissue is damaged. While they are a normal response to injuries such as cuts, burns, acne, or surgery, many people prefer to reduce their appearance or prevent them from forming in the first place.
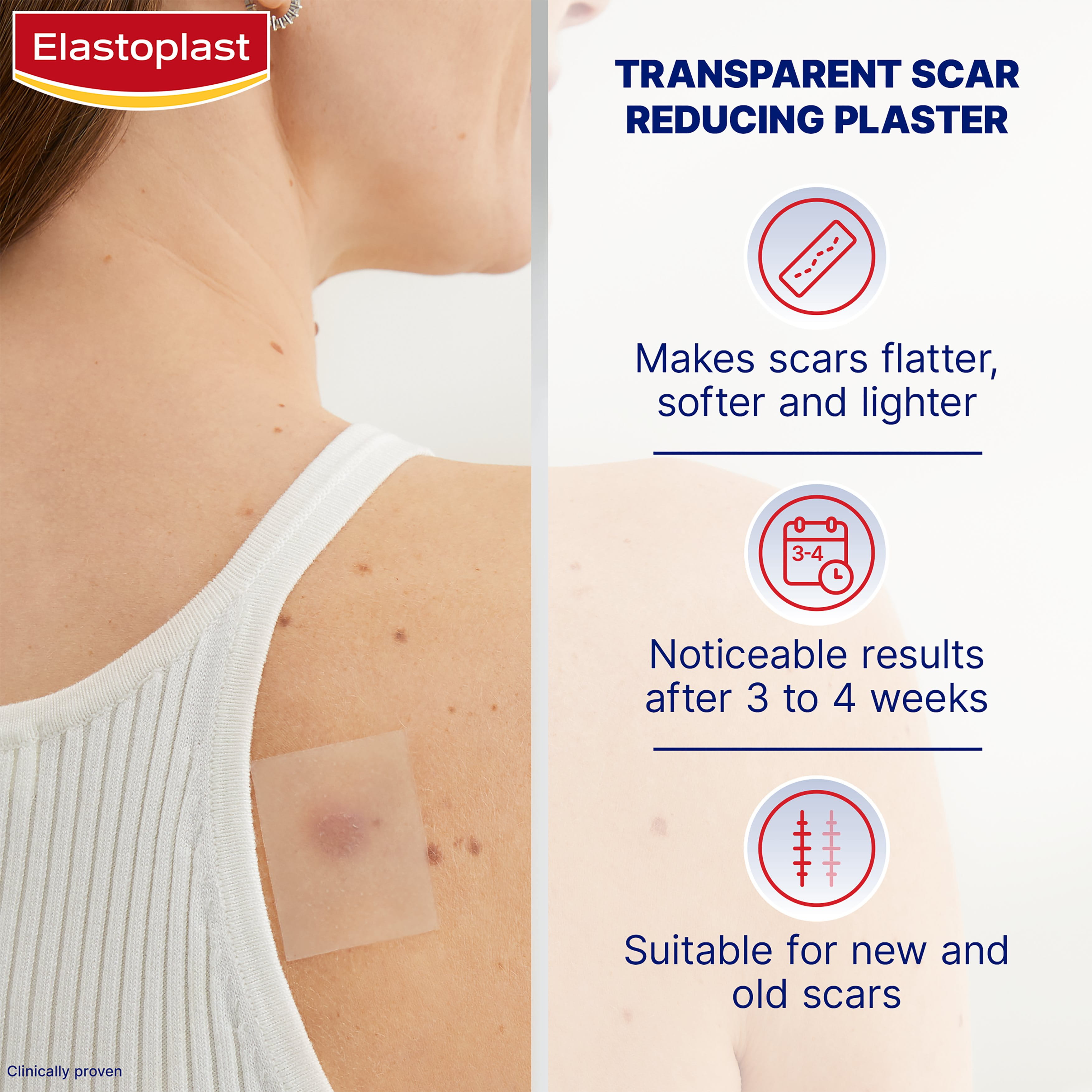
Proper care during and after wound healing can significantly affect how a scar looks over time. Using Elastoplast products such as Scar Reducer Plasters, Hydrocolloid Plasters, Wound Spray, and Wound Healing Ointment can support the healing process, protect the skin, and help reduce visible scarring. Learn more below about how to prevent scars from forming and reduce their visibility.